AI-Powered Prior Authorization—Unified Across Medical & Pharmacy
PAHub™ is a CMS-0057–ready solution that uses advanced AI automation to streamline medical and pharmacy prior authorizations, reducing resource-intensive workflows, improving operating costs, saving time, improving member satisfaction, reducing provider abrasion and ultimately reducing avoidable delays in care.


Efficiency Across Both Benefits
Delivering Automated & AI-Powered Prior Authorization for Medical & Pharmacy
The complexity of prior authorization, spanning both pharmacy and medical benefits, continues to intensify, driving up costs and placing increasing pressure on health plans and PBMs to manage speed, accuracy, and compliance at scale. PAHub delivers a smarter, more modern approach, leveraging advanced AI-driven automation to transform how prior authorization is managed from intake through final decision.
Purpose-built to address rising volumes and increasingly complex clinical criteria, PAHub applies intelligent document processing, automated criteria extraction, and dynamic decision logic to streamline end-to-end workflows to prevent delays in care. The result is faster, more consistent decisions, strengthened compliance, and a meaningful reduction in administrative burden, without compromising clinical integrity.
As a HITRUST-certified platform, PAHub enables organizations to scale prior authorization operations with confidence. By reducing friction across the process, it accelerates turnaround times, lowers administrative costs, and delivers a more efficient, seamless experience for providers and members alike.


All Lines of Business
Supported across all lines of business (commercial, exchange, Medicare, Medicaid, etc)
All Channels
Available across all channels (electronic prior authorization (ePA), phone, fax, web, etc.)
All Healthcare Services
Applicable for all healthcare services, all benefit types (pharmacy, medical Rx and medical procedures)
Calculate Your ROI By Using PAHub
Wondering how much time and money PAHub could save your team? Complete the following form.
PAHub’s Key Capabilities:
Leveraging Advanced Intelligence
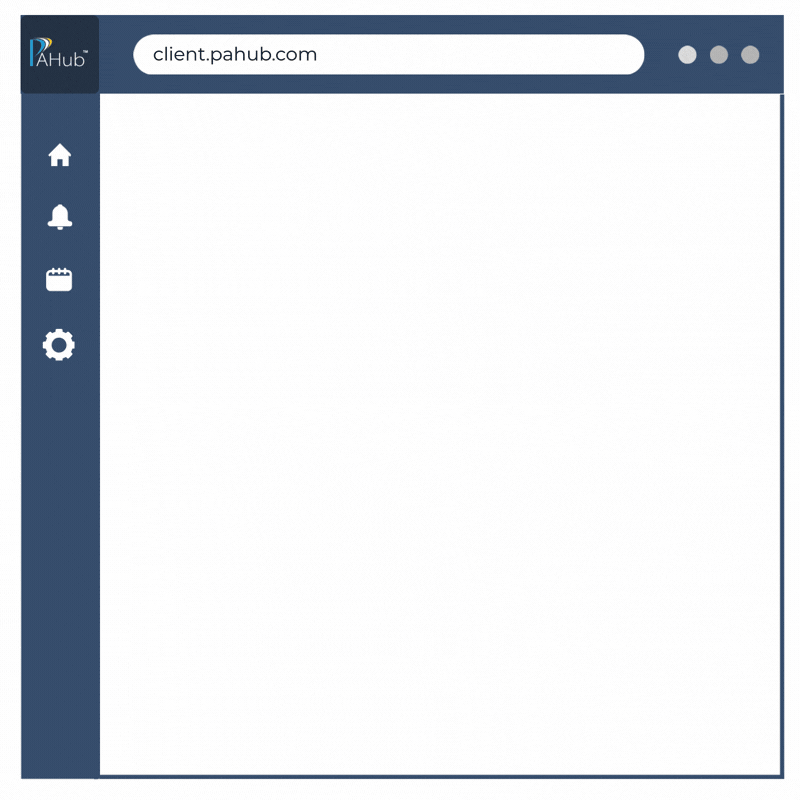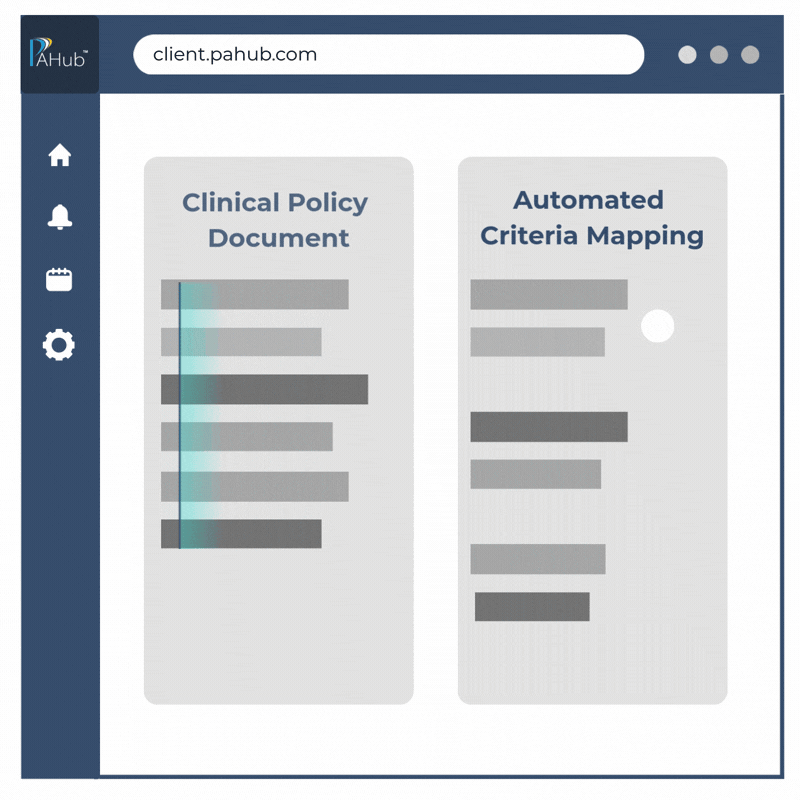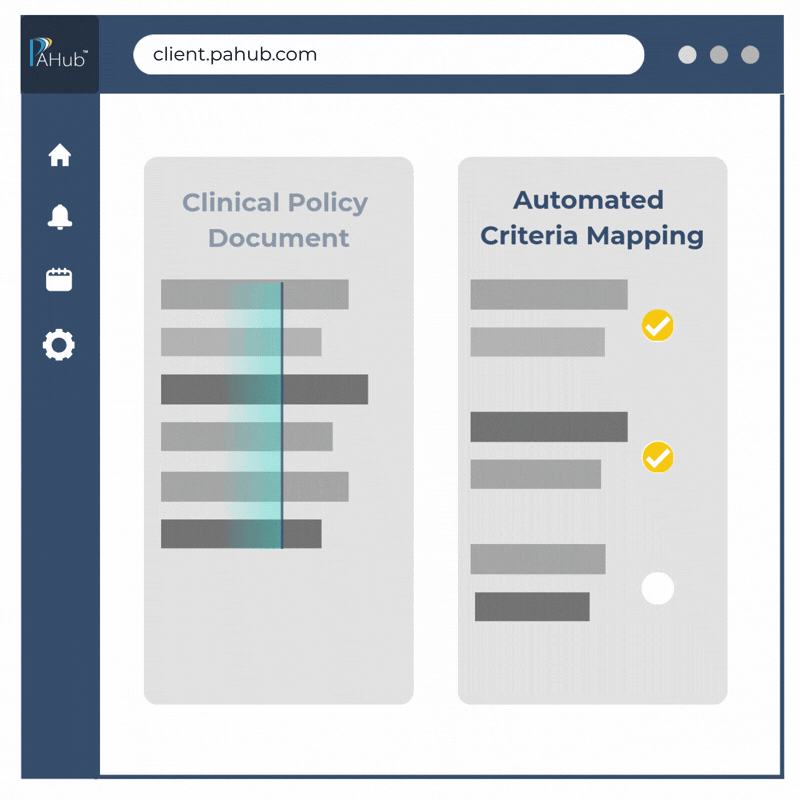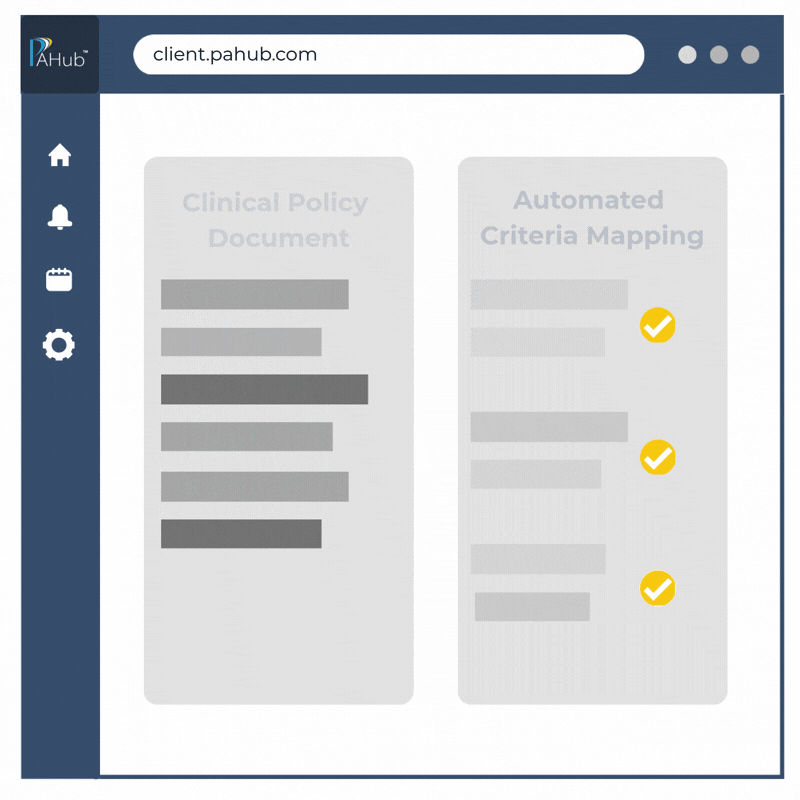
CriteriaBuilder: Clinical Criteria Build Automation
Turn Clinical Guidelines into Actionable Criteria in Seconds—Automatically with CriteriaBuilder.
Medical policies and clinical criteria aren’t simple anymore. Neither are drug requests. Our CriteraBuilder tool is designed to handle today’s most complex utilization management scenarios—automatically, accurately, and at scale. We transform any clinical criteria, including but not limited to CMS Guidelines, MCG, InterQual, payer specific medical policies, into structured clinical question sets, decision paths, and approval workflows. We automate manual processes while improving consistency and accuracy.
Criteria Builder in PAHub streamlines the creation and maintenance of clinical rules by converting guidelines and policy into digitized and codified criteria with speed and accuracy. Codifying clinical criteria takes minutes, not days. This means customers are now able to optimize CMS-0057 and interoperability clinical record exchange opportunities.
ClinIntel: Intelligent Data Extraction & Clinical Automation
Transform Unstructured Clinical Data into Actionable Intelligence
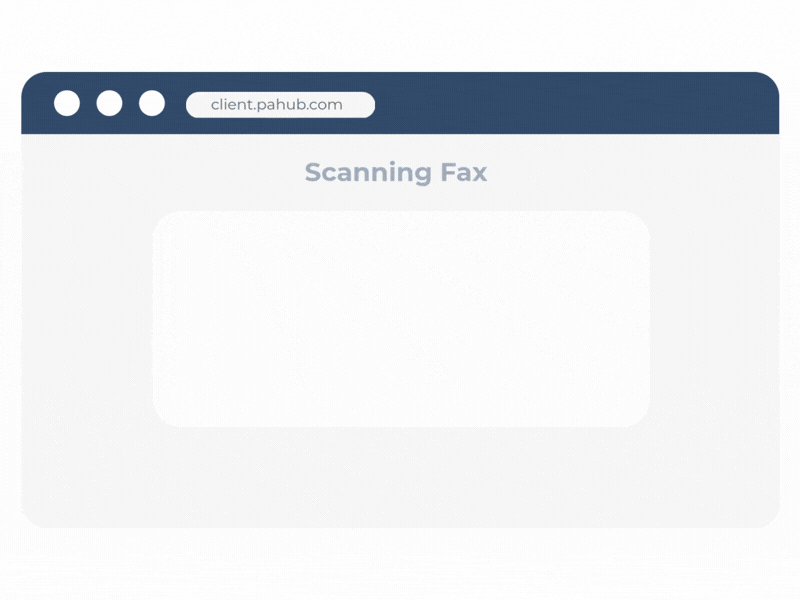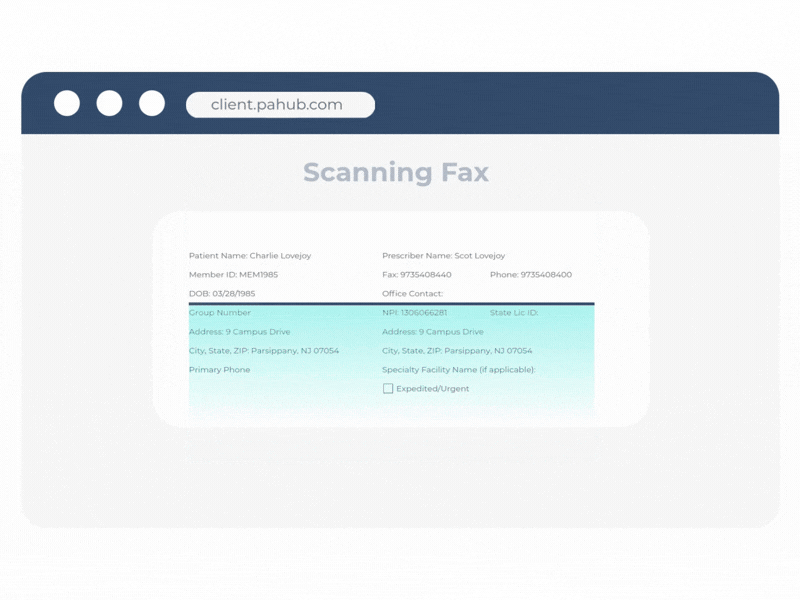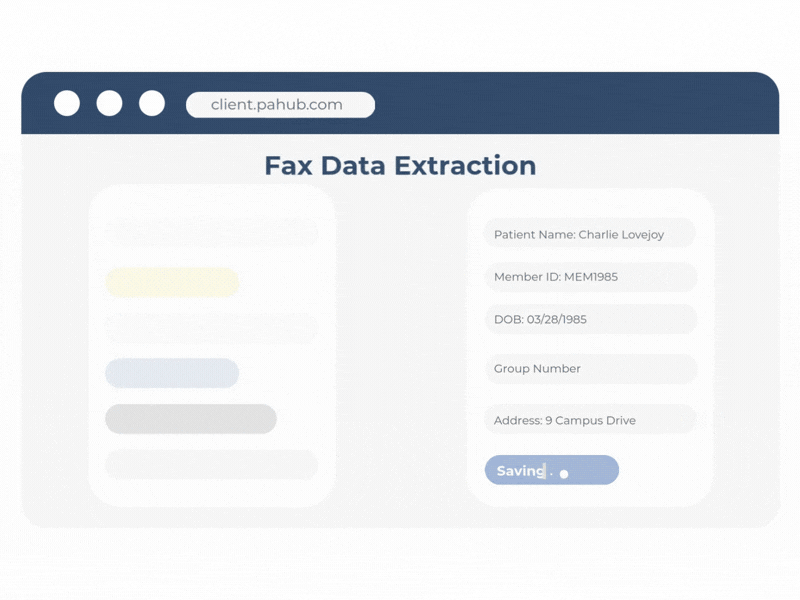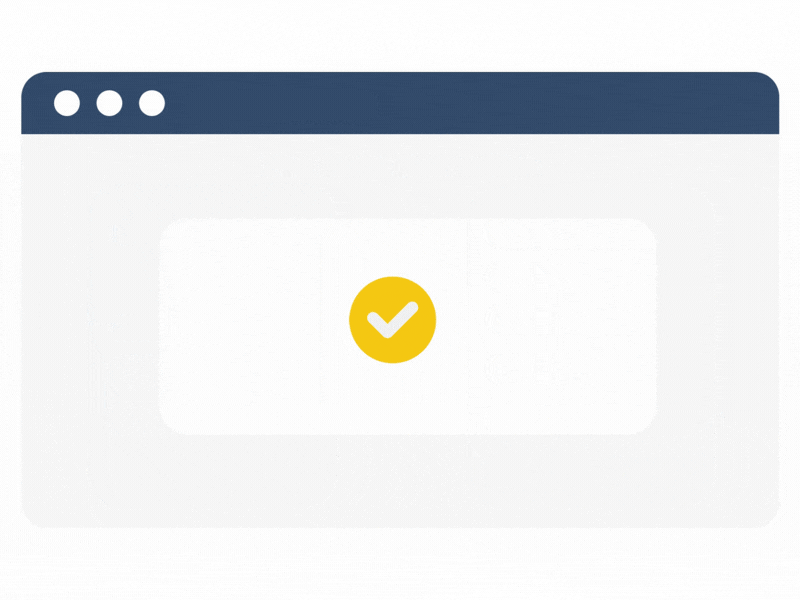
ClinIntel, part of the PAHub platform, converts unstructured clinical information into structured, actionable data—automatically. Building on Agadia’s proven Fax Data Extraction (FDE) capabilities, ClinIntel leverages advanced OCR and intelligent document processing to capture key data from incoming faxes, attachments, and clinical documentation.
ClinIntel can extract and normalize information from a wide range of sources, including faxed forms, uploaded documents, and electronic medical records (when EHR connectivity is enabled). The platform identifies critical clinical and administrative fields, validates the data, and routes it seamlessly into PAHub workflows and downstream systems.
ClinIntel is advancing beyond traditional data extraction to power clinical decision automation—enabling organizations to fundamentally transform prior authorization and utilization management. By driving faster, more accurate decisions at scale, ClinIntel reduces administrative friction, accelerates workflows, and elevates operational performance across the enterprise.
Auto Decision Capabilities
Faster Decisions Through Intelligent Automation
PAHub’s Auto Decision capabilities deliver fast, consistent authorization decisions by automatically evaluating requests against configured clinical and administrative rules. By making real-time approvals and denials for a clinician to review, PAHub reduces manual review, shortens turnaround times, and ensures decisions are applied accurately and consistently—at scale.
CMS-0057 Ready
Positioned to Help Payers Navigate the CMS Interoperability & Prior Authorization Final Rule
Built to support FHIR-based prior authorization workflows, PAHub enables standardized data exchange, faster decisioning, and improved transparency across the authorization lifecycle. With automation, real-time status tracking, and seamless integration into existing clinical and administrative systems, PAHub helps organizations reduce manual effort, accelerate turnaround times, and meet CMS-0057 requirements while delivering a better experience for both providers and members.

PAHub Insights
Actionable Intelligence for Smarter Prior Authorization Decisions
PAHub Insights delivers real-time visibility into prior authorization performance, empowering health plans and PBMs with the data they need to continuously optimize operations. By transforming prior authorization activity into actionable analytics, PAHub Insights highlights trends across volume, turnaround time, approval outcomes, and clinical pathways—across both the pharmacy and medical benefit. With intuitive dashboards and AI-driven insights, organizations can identify bottlenecks, monitor compliance, and make informed decisions that improve efficiency, consistency, and overall prior authorization outcomes.
Engage Pharmacies, Members & Providers
In the Prior Authorization and Pre-Certification Process
PromptPA is a self-service, web-based solution that enables our customers’ providers, facilities, pharmacies, and members to request electronic prior authorization, initiate renewals, and check the status of requests using any web browser, reducing operational costs and call volume to Health Plans and Benefit Managers.
PromptPA can also be leveraged by Hubs, Specialty Pharmacies and Drug Manufacturers to streamline the prior authorization process and ensure quick and accurate access to care.
Quick Facts
Lives Covered Across Customer Base
Health Plan & Pharmacy Benefit Management (PBM) & Third-Party Administrator (TPA) Customers
Prior Authorizations Processed Annually
%
Electronic Prior Authorizations Processed
Why Choose Agadia for your
Medical Prior Authorization Needs
Comprehensive and Configurable
Full control to configure clinical, operational, and compliance rules.
Seamlessly supports all CPT and HCPCS codes, ensuring compatibility across all categories, including radiology, musculoskeletal, DME, lab, surgery, and behavioral health.
Tailored workflows to meet delegated and non-delegated requirements.
Built for Compliance
Proven track record of supporting CMS audits for over 13 years.
Ready for CMS 0057-F compliance, with integrated solutions for InterQual, CMS, and custom criteria.
Cutting Edge Technology
Real-time integration with claims systems for efficient automation and decision-making.
Advanced AI and NLP capabilities to reduce manual intervention and improve accuracy.
8-9 enhancement releases annually to ensure your solution stays ahead of the curve.
Automation at Scale
Auto-decisioning and ePA capabilities for faster approvals.
Customizable letter generation and communication management tools to reduce administrative burden.
Clinical data extraction and EMR integration for next-gen functionality.
Continually Innovating to Meet Industry Needs
Addressing Electronic Prior Authorization for Drugs Under the Medical Benefit
As more infused and specialty medications are administered in physician offices, prior authorization for drugs billed under the medical benefit has become increasingly challenging across the industry. While there is a well-established electronic prior authorization (ePA) standard for pharmacy benefit drugs, no comparable industry standard exists today for medical benefit medications.
Unlike pharmacy benefit drugs, medical benefit medications are often purchased directly by providers from distributors and administered in the office or infusion center. Because these drugs don’t follow the traditional e-prescribing and pharmacy fulfillment workflow, health plans still receive many medical benefit prior authorization requests by phone, fax, or portal. This creates significant administrative burden for health plans, provider offices, and patients—and often leads to delays in care.
Agadia addresses this gap with electronic Medical Prior Authorization (eMPA) capabilities that streamline and automate medical benefit prior authorizations. By creating a more efficient digital pathway, Agadia helps reduce manual work, improve turnaround times, and clearly identify whether a drug falls under the pharmacy or medical benefit. Providers receive faster answers, hub partners gain operational efficiencies, and patients benefit from quicker access to therapy and improved adherence.

An ironclad compliance strategy
Setting the benchmark for industry standards and best practices
PAHub incorporates Continuous Compliance Surveillance Channels, allowing us to proactively align with industry leaders in the Medicare space and ensure ongoing adherence to regulatory requirements.
Health Plans and PBMs can confidently rely on PAHub from a compliance standpoint. With a deep understanding of regulatory requirements and extensive experience and partnerships in the healthcare industry, Agadia enables clients to adhere to Medicare Part D guidelines while maintaining data integrity and accuracy.










