AI-Powered Prior Authorization—Unified Across Medical & Pharmacy
PAHub™ is a CMS-0057-ready prior authorization solution that uses advanced automation to streamline medical and pharmacy prior authorizations, reduce manual workflows, improve turnaround times, and support a better provider and member experience.

Delivering automated and AI-powered prior authorization for medical and pharmacy.
The complexity of prior authorization across pharmacy and medical benefits continues to intensify, driving up costs and increasing pressure on Health Plans and PBMs to manage speed, accuracy, and compliance at scale.
PAHub delivers a smarter approach by applying intelligent document processing, automated criteria extraction, configurable decision logic, and connected workflows from intake through final decision.
As a HITRUST-certified platform, PAHub helps organizations scale prior authorization operations with confidence while improving provider and member experience.
Leveraging advanced intelligence across the full PA lifecycle.
Each PAHub capability helps automate a different part of the prior authorization process, from clinical criteria buildout to intelligent data extraction, decisioning, reporting, and provider engagement.
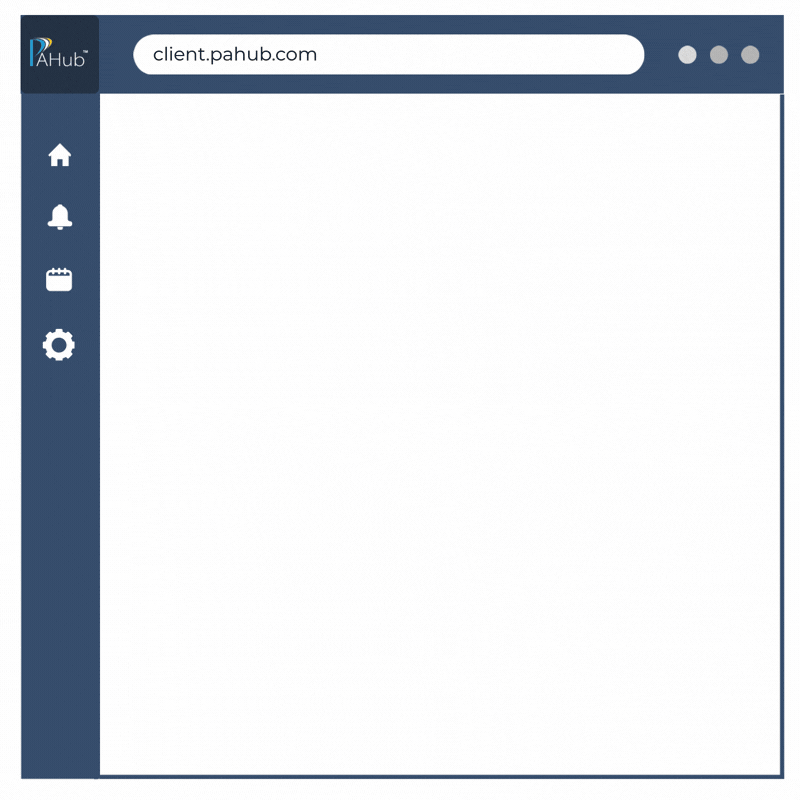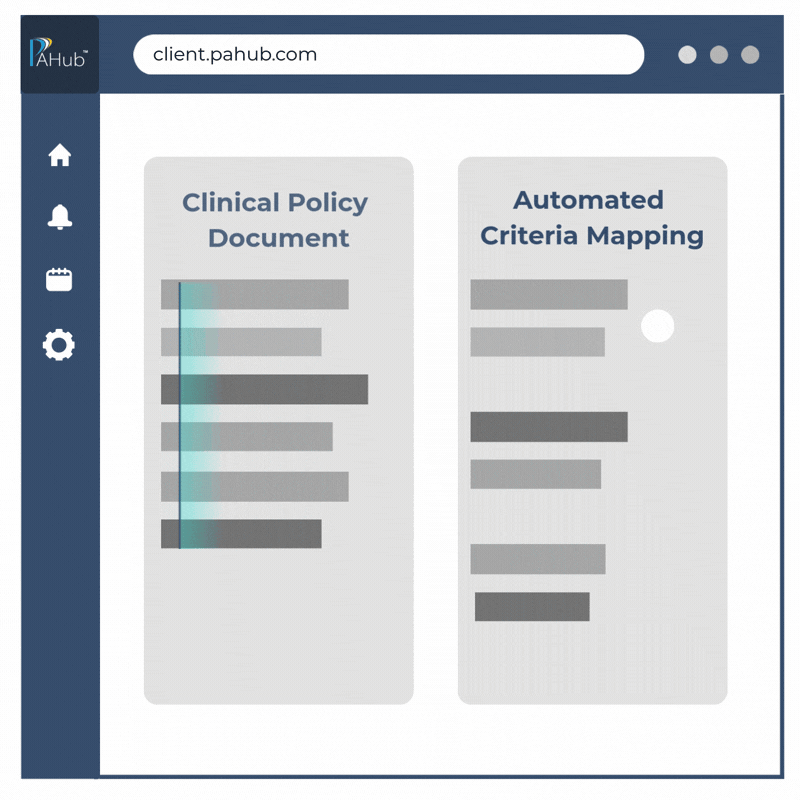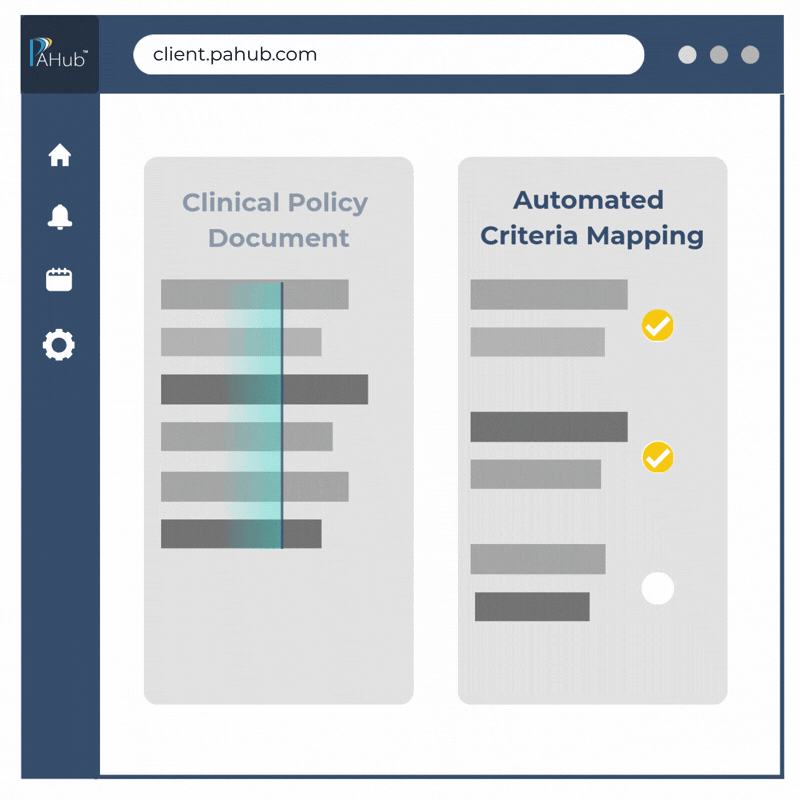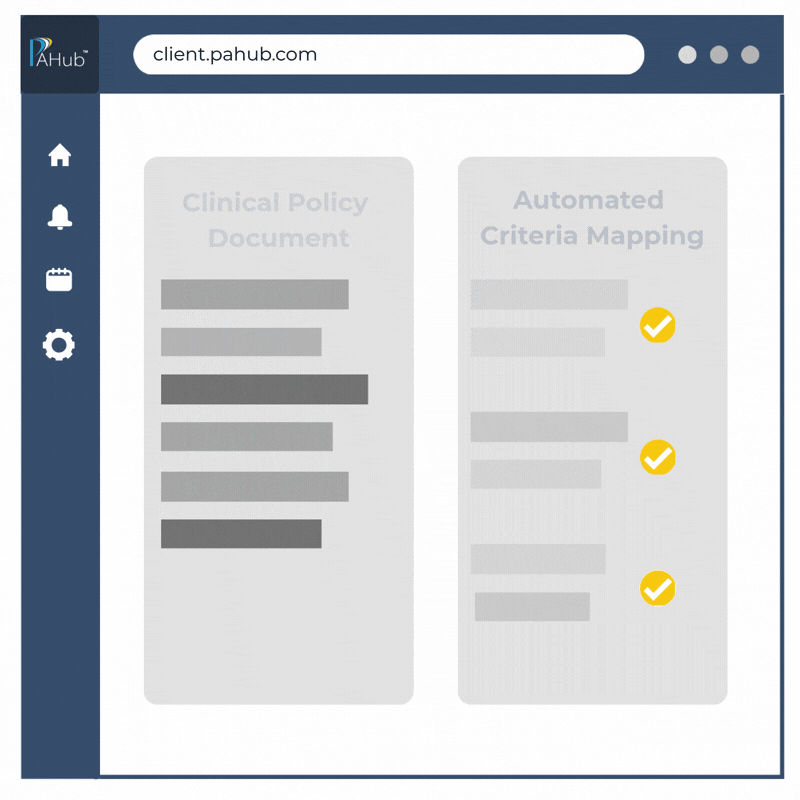
Turn clinical guidelines into actionable criteria in seconds.
CriteriaBuilder converts guidelines and medical policies, including CMS Guidelines, MCG, InterQual, and payer-specific criteria, into structured clinical question sets, decision paths, and approval workflows.
Codifying clinical criteria takes minutes, not days, helping customers optimize clinical record exchange and support CMS-0057 interoperability opportunities.
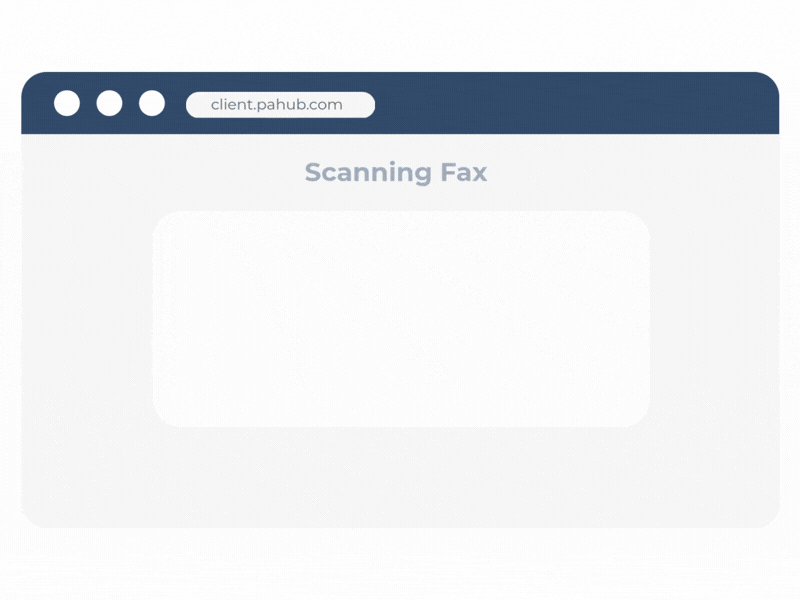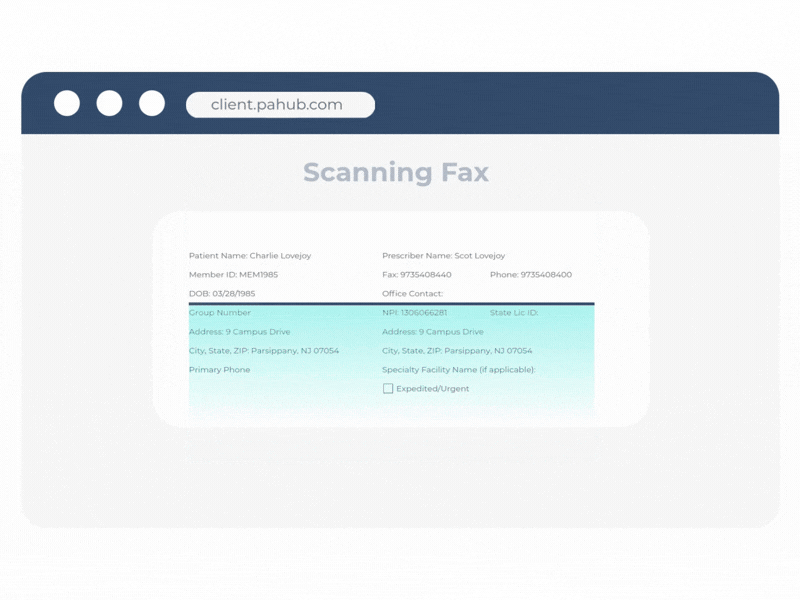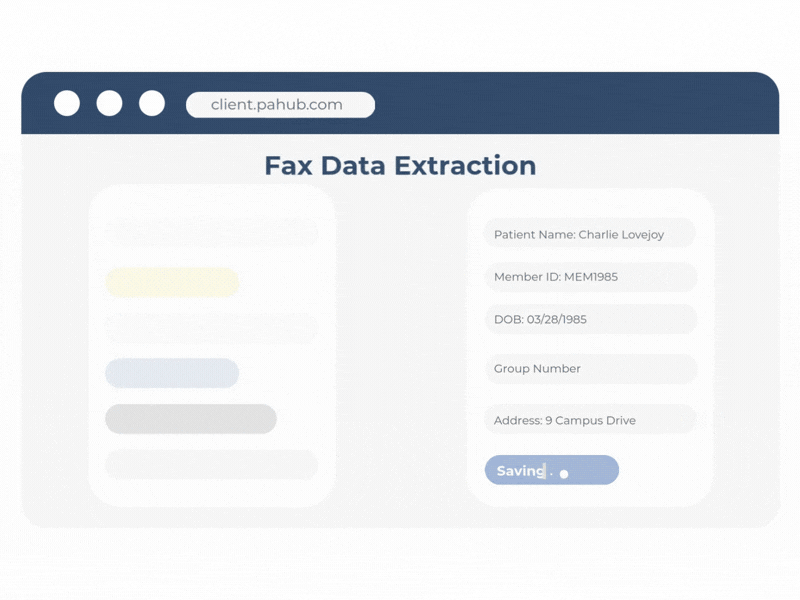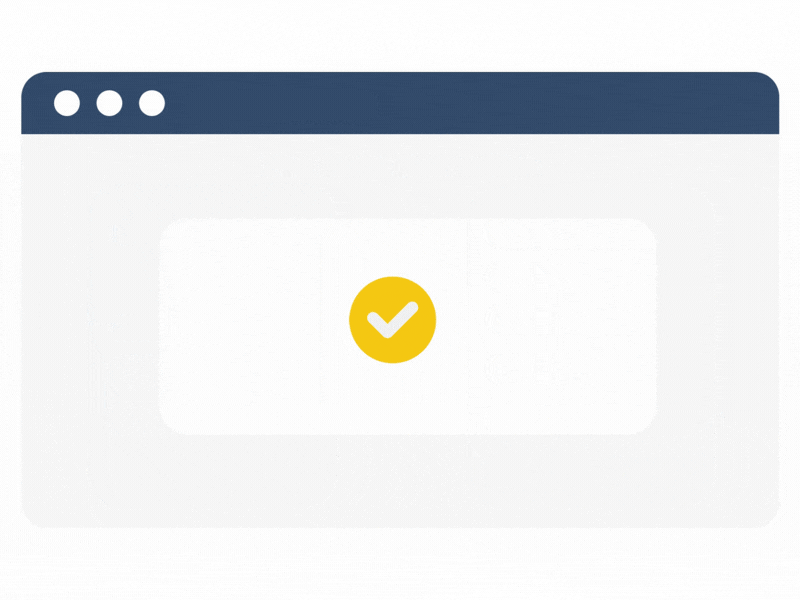
Transform unstructured clinical data into actionable intelligence.
ClinIntel converts unstructured clinical information into structured, actionable data. It builds on Agadia’s Fax Data Extraction capabilities to capture key data from faxes, attachments, uploaded documents, and clinical records when EHR connectivity is enabled.
By routing normalized data into PAHub workflows, ClinIntel helps reduce administrative friction, accelerate workflows, and power clinical decision automation.
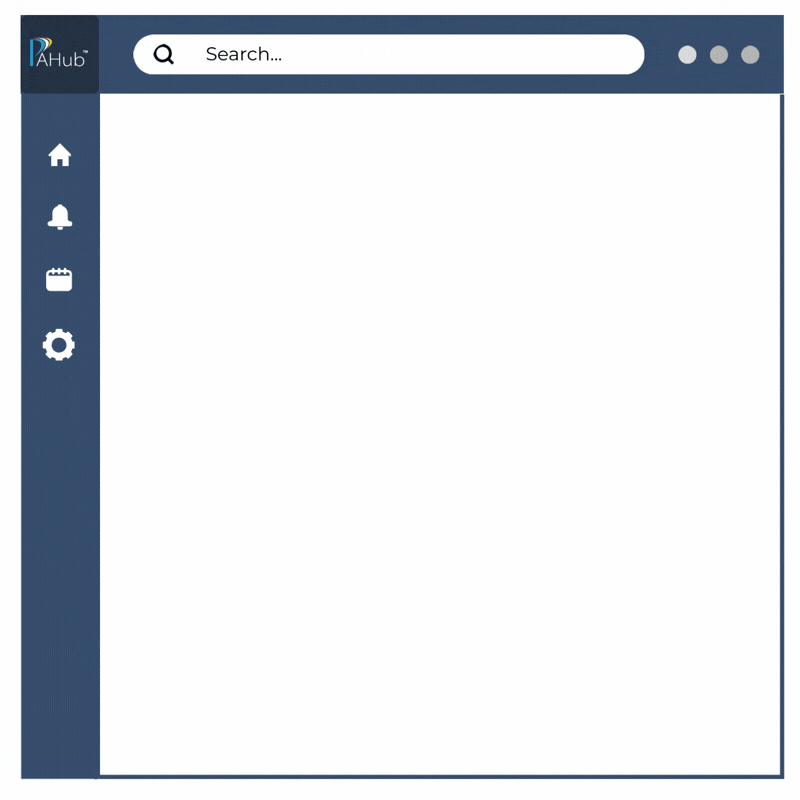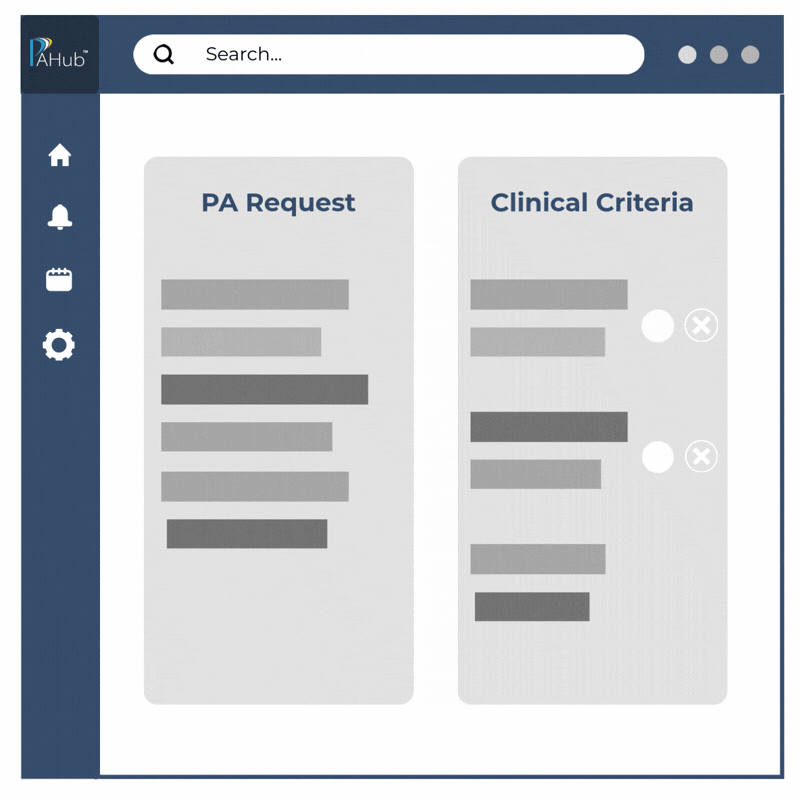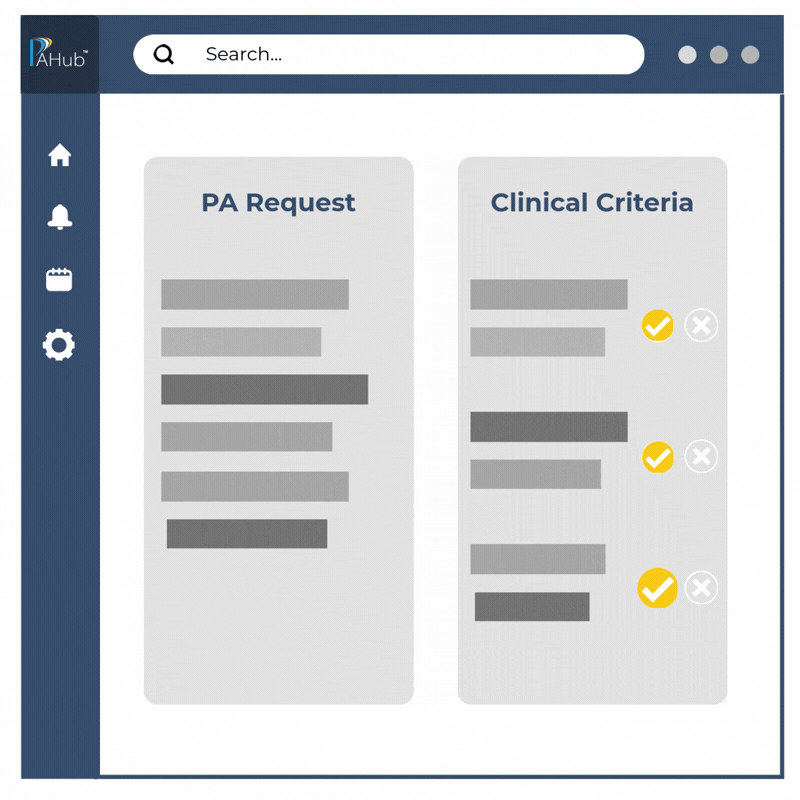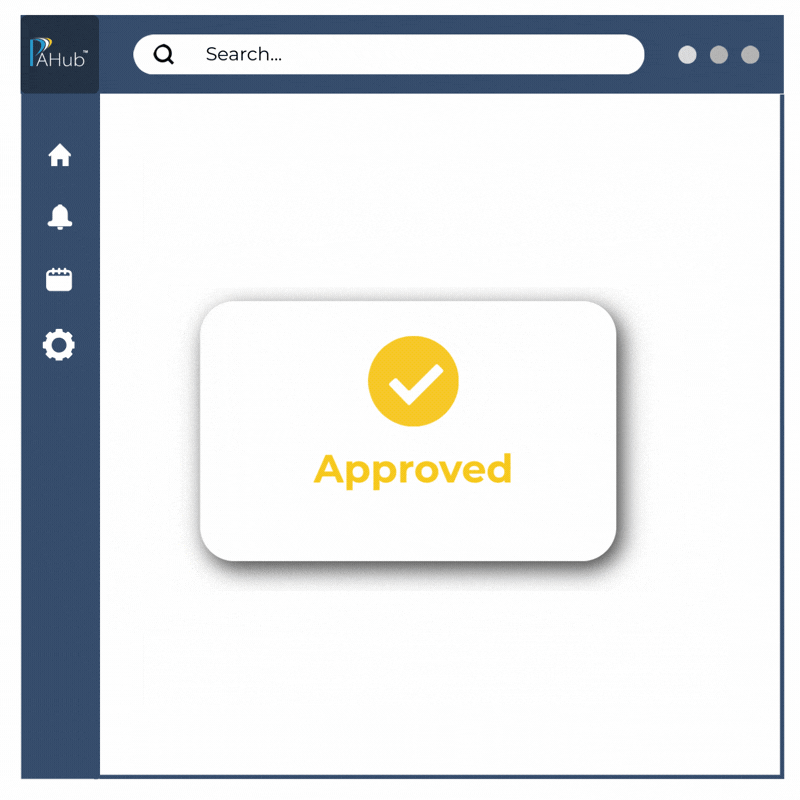
Faster decisions through intelligent automation.
PAHub’s Auto Decision capabilities evaluate authorization requests against configured clinical and administrative rules to help deliver fast, consistent, and accurate outcomes at scale.
By automating eligible approvals and routing complex requests to the right reviewer, PAHub reduces manual review, shortens turnaround times, and strengthens decision consistency.

Positioned to help payers navigate CMS interoperability and prior authorization requirements.
PAHub supports FHIR-based prior authorization workflows, standardized data exchange, faster decisioning, status tracking, and improved transparency across the authorization lifecycle.
With automation and integration into existing clinical and administrative systems, PAHub helps organizations reduce manual effort, meet interoperability expectations, and deliver a better experience for providers and members.
Actionable intelligence for smarter prior authorization decisions.
PAHub Insights delivers real-time visibility into PA performance, helping Health Plans and PBMs track volume, turnaround time, approval outcomes, clinical pathways, bottlenecks, and compliance trends across pharmacy and medical benefit workflows.
Intuitive dashboards and AI-driven insights help teams make informed decisions that improve efficiency, consistency, and outcomes.
Engage pharmacies, members, providers, and facilities through PromptPA—connected directly into PAHub.
PromptPA is the front-door portal experience that allows users to submit requests, initiate renewals, upload documentation, and check status from any web browser. Those requests flow into PAHub, Agadia’s industry-leading prior authorization solution for Health Plans and PBMs.
PromptPA Portal
Providers, facilities, pharmacies, and members submit requests, renewals, attachments, and status checks.

PAHub Platform
PAHub applies criteria, automation, routing, decisioning, notices, reporting, and audit-ready documentation.
Proven scale for Health Plans and PBMs.
Built for complex medical and pharmacy prior authorization needs.
PAHub helps Health Plans and PBMs manage prior authorization with configurable workflows, compliance support, automation at scale, and continuous innovation.
Comprehensive & Configurable
- Full control over clinical, operational, and compliance rules.
- Support for CPT and HCPCS categories including radiology, DME, lab, surgery, and behavioral health.
Built for Compliance
- Proven CMS audit support.
- CMS-0057-F readiness with clinical criteria and interoperability support.
Cutting-Edge Technology
- Real-time integration with claims and clinical systems.
- AI and NLP capabilities to reduce manual intervention.
Automation at Scale
- Auto-decisioning and ePA workflows.
- Letter generation, communication management, and EMR integration.

Addressing electronic prior authorization for drugs under the medical benefit.
As more infused and specialty medications are administered in physician offices, prior authorization for drugs billed under the medical benefit has become increasingly challenging.
Agadia helps close this gap with electronic Medical Prior Authorization capabilities that streamline and automate medical benefit authorizations, reduce manual work, improve turnaround times, and clarify whether a drug falls under the pharmacy or medical benefit.
Explore the potential benefits you can achieve with PAHub.
The following case studies reveal how Health Plans and PBMs have leveraged PAHub to increase PA volume, expand ePA adoption, improve efficiency, support compliance, and reduce FTE burden.