Electronic Prior Authorization Process & Automation Software
Improve Clinical Efficiency & Compliance with Agadia’s fully customizable web-based solution, PAHub™.


Delivering Electronic Prior Authorization Efficiency & Compliance
As Prior Authorization volumes continue to rise, and as specialty drugs create additional clinical complexities, Health Plans, Pharmacy Benefit Managers (PBMs) and Third-Party Administrators (TPAs) are challenged to adapt while maintaining or improving operational and clinical efficiencies. PAHub, is a HITRUST certified solution that puts the tools at your fingertips to streamline and control all clinical, compliance and administrative aspects of Prior Authorization at the point-of-care to improve compliance, reduce turn-around times and costs.
By leveraging the latest technologies for data mining, data analytics, content management and advanced decision support trees, PAHub, enables customers to automate the end-to-end prior authorization process.
All Lines of Business
Supported across all lines of business (commercial, Medicare, Medicaid, etc.)
All Channels
Available across all channels (electronic prior authorization (ePA), phone, fax, web, e-prescribing, etc.)
All Healthcare Services
Applicable for all healthcare services, all benefit types (pharmacy & medical)
A Centralized Prior Authorization Solution
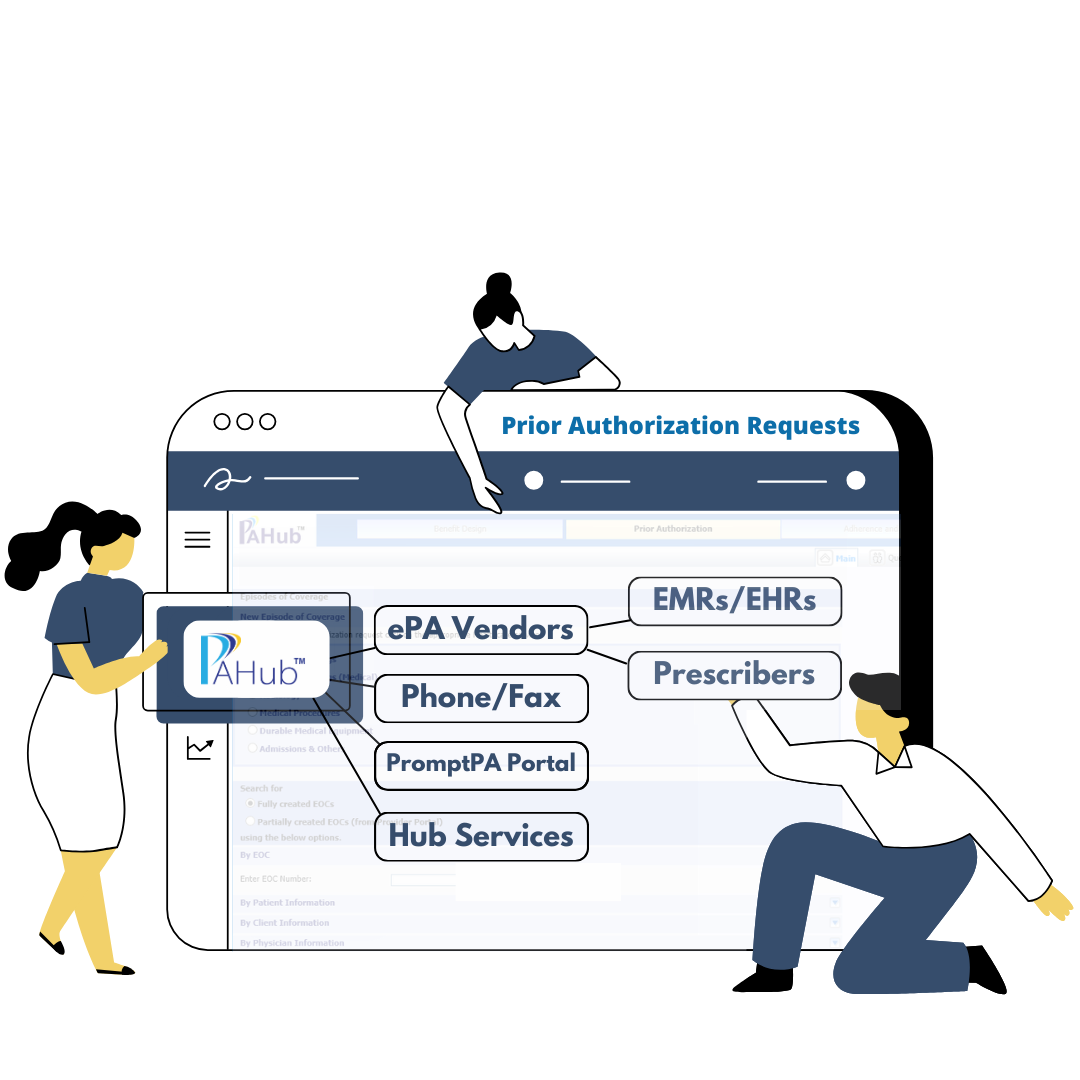
Continually Innovating to Meet Industry Needs
Addressing Electronic Prior Authorization for Drugs Under the Medical Benefit
With an influx of infused medications being administered in physician offices, prior authorizations for drugs billed under the medical benefit are presenting challenges across the industry. While there is an industry NCPDP SCRIPT standard for electronic prior authorization (ePA) for drugs billed under the pharmacy benefit, driving significant ePA volume, an industry standard does not currently exist for drugs under the medical benefit.
The challenge with adopting the NCPDP SCRIPT standard for drugs under the medical benefit is that these medications typically do not go the standard route of provider e-prescribing to a traditional retail or mail-order pharmacy location. Often times, the specialty medications are being purchased by the provider (physician/infusion center) directly from drug distributors and administered in the office setting. As a result, health plans continue to receive the drugs under the medical benefit prior authorization requests via phone, fax, or portal which is placing an enormous administrative burden on the health plans operations team, provider office, and the patient.
Agadia continues to innovate and has addressed these challenges by providing eMPA capabilities to reduce the prior authorization administrative burden through a more efficient channel that increases automation and improves turnaround times. Providers will benefit by quickly being informed whether the drug is under the pharmacy or medical benefit, allowing them to efficiently manage requests. Hub companies will experience improved efficiencies as well such as faster turnaround times for a prior authorization decision, improved patient speed to therapy and better adherence.
Leverage Advanced Technologies
QuickPA
QuickPA delivers a new level of automation and efficiency to PAHub. With this enhancement, PAHub will further reduce manual processes, minimize user clicks, and streamline the end-to-end management of a PA.
How You’ll Benefit:
- Increased Efficiency: QuickPA automates the PA creation process with intelligent selection, reducing the number of manual steps and clicks needed.
- Improved User Experience: The modern UI/UX design provides a user-friendly interface, making it easier for users to navigate, complete, and review PA requests.
- Enhanced Document Management: Unlock further efficiencies when integrating with PAHub’s Fax Data Extraction feature, which leverages machine learning and NLP technologies that go beyond traditional ICR and OCR to extract key data from incoming faxes, reducing manual data entry and improving data accuracy.
- Consistency & Accuracy: By guiding users to enter essential information and automating the selection process, QuickPA helps create standardized PA requests.
- Real-Time Data Access: The QuickPA toolbar allows users to access key information about the PA request without leaving the summary page.
- Streamlined Communication: Display informative messages and alerts to guide users and highlight any missing or essential information.
Auto-Decision
PAHub’s Auto-Decision rules engine increases automation be leveraging data mining techniques across enterprise systems data to electronically adjudicate prior authorization requests. Auto-Decision helps a customer to allocate staff to high-touch requests instead of requests that can be adjudicated automatically.
PAHub Insights
Experience a pivotal enhancement to your prior authorization management experience with PAHub Insights. Reshape your reporting to transform data into actionable insights. How you’ll benefit:
Rich Visual Dashboards: Gain unprecedented operational and managerial insights to help make data-driven business decisions.
Interactive Capabilities: Interactive reports are the future of data analysis. With drill-down and drill-through capabilities, you can explore data on a granular level. Uncover trends, identify anomalies, and take immediate action.
Self-Service Ad Hoc Reporting: Empower your team with self-service reporting. This self-service functionality streamlines your operations, giving your team the tools to stay agile and responsive.
Increased Productivity: Gain valuable insights into the PA creation process, allowing you to optimize user workflows, identify trends, and streamline sign-off procedures.
Informed Decision Making: Elevate your strategic decision-making with access to a high-level view of your data landscape and the ability to analyze PA volume across various parameters.
Fax Data Extraction
By leveraging machine learning and NLP technologies that go beyond traditional ICR and OCR, Health Plans & PBMs can now extract key information from incoming faxes and convert to structured digital data within PAHub.
Streamlined Document Management & Page Tagging: Experience an enhanced document management process on an improved user interface that simplifies user interactions, data validation, page tagging and minimizes fax touch time.
Automated Data Extraction: Extract key attributes from the fax image, such as patient details, drug information, prescriber details, provider information, and any handwritten notations, while automatically performing eligibility lookups for multi-patient recognition.
Save Valuable Time: Effortlessly capturing vital details from incoming faxes not only saves valuable time but elevates the user experience. This streamlined process not only facilitates more informed decision-making but also ensures timely actions, resulting in better member outcomes.
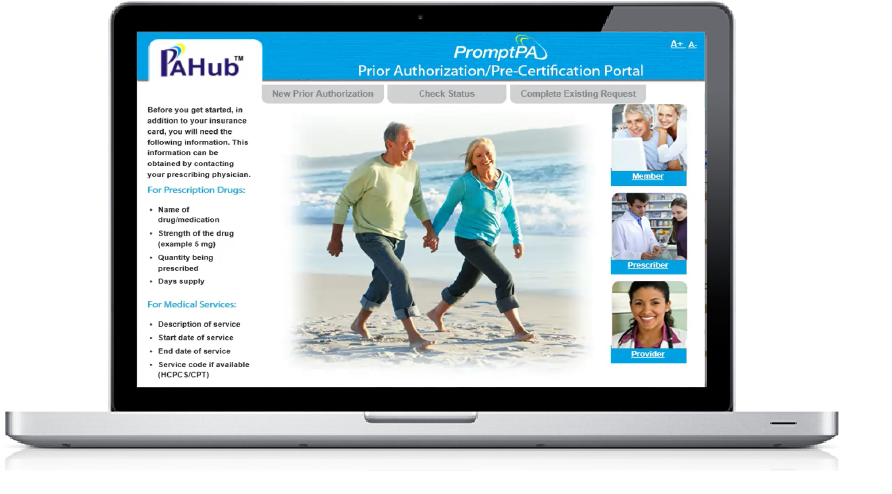
Engage Pharmacies, Members & Providers
In the Prior Authorization and Pre-Certification Process
PromptPA is a self-service, web based solution that enables our customers’ pharmacies, members and providers to request prior authorizations electronically, initiate renewals and check the status of requests using any web browser, reducing operational costs and call volume to Health Plans and Benefit Managers.
An ironclad compliance strategy
Setting the benchmark for industry standards and best practices
PAHub incorporates Continuous Compliance Surveillance Channels, allowing us to proactively align with industry leaders in the Medicare space and ensure ongoing adherence to regulatory requirements.
Health Plans and PBMs can confidently rely on PAHub from a compliance standpoint. With a deep understanding of regulatory requirements and extensive experience and partnerships in the healthcare industry, Agadia enables clients to adhere to Medicare Part D guidelines while maintaining data integrity and accuracy.
Industry Accedidations Followed:
State & Federal Agencies:
Quick Facts
Lives Covered Across Customer Base
Health Plan & Pharmacy Benefit Management (PBM) & Third-Party Administrator (TPA) Customers
Prior Authorizations Processed Annually
%
Electronic Prior Authorizations Processed
Phone
877-575-2533
contact@agadia.com
Location
9 Campus Drive, Parsippany NJ 07054
© 2025 Agadia Systems, Inc. All Rights Reserved.
Legal Information | Sitemap